Cure4CF Update
From Defense to Damage: The Surprising Role of Mucus in Bronchiectasis
Professor Jodie Simpson, Head of Research, Cure4CF
What is mucus?
Mucus is a protective, gel-like substance found throughout the body, where it traps germs, lubricates tissues, and helps keep organs like the lungs, gut, and reproductive system functioning properly.
If you don’t have CF, you might only notice mucus in your lungs when you have a cold or a chest infection. You might to start to cough up mucus or phlegm; it can change colour from clear to opaque (white like) to yellow to green. Mucus changes when we are sick, especially when we have been infected with a virus or bacteria.
If you notice that the mucus you are spitting up is colour 4 or 5 on the Bronkotest card– you most definitely have some important white blood cells called neutrophils trying to fight something off in your lungs. This colour can also suggest you might need antibiotics!

Did you know that the colour of your mucus can tell you about the type of inflammation and possible infection you might have?
Mucus is vital and understanding it can help us understand our lungs.
For people with CF, the type of mucus others experience once or twice a year when they have a cold is often present all the time.
The differences in the CFTR gene mean that the changes that occur in chloride transport also impact the mucus in the body – including the lungs.
In CF the differences in the mucus can mean that infections are often not as easily cleared and airway damage can result. The damage that can occur is called Bronchiectasis – this is when the airways become enlarged and filled with mucus. Once you reach adulthood the airways can become permanently enlarged and cannot be changed.
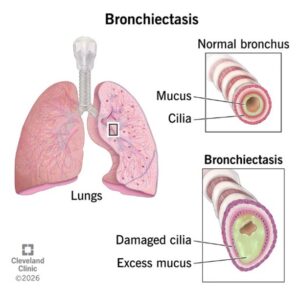
What is the role of mucus in bronchiectasis?
This month I caught up with the winner of the first Cure4CF and Lung Foundation Australia World Bronchiectasis Travel Award.
Crystal Bourke is a Senior Physiotherapist at the Perth Children’s Hospital and a PhD Candidate at The Kids Research Institute and the University of Western Australia. Crystal works with children with CF and another important rare lung disease, primary ciliary dyskinesia (PCD). These conditions have something in common – they are both very prone to develop bronchiectasis. Australian data suggests that by 3 years of age, around 60% of children with CF already have evidence of bronchiectasis. Several reports also suggest that people who are CF carriers, may be at a higher risk of also having bronchiectasis. Indeed, people who have bronchiectasis and are a CF carrier are more likely to have Pseudomonas and NTM infections, experience hospitalisations and require more antibiotics than people who have bronchiectasis and do not have a CF gene (doi: 10.1093/ofid/ofae024). This means even having one copy of the CF gene and bronchiectasis can impact your lung health.
Crystal explained that the mucus and inflammation in CF is more severe than in PCD. While CF modulator treatment can improve the mucus in people with CF, the mucus is still different to people who do not have CF. The team in Perth are working to understand mucus in bronchiectasis, and they have found that it is hyperconcentrated. The more hyperconcentrated the mucus, the more respiratory symptoms children experience, and these children have often had bronchiectasis for longer.

Mucus hyperconcentration means the mucus is extra thick and sticky because it does not have enough water. The team are working to understand how mucus is different in children with bronchiectasis. Crystal explained if they can identify when and why the changes in mucus happen, then it may be possible to prevent the changes and ultimately prevent bronchiectasis. Studying this in children is vital, before changes become permanent and irreversible.
The data so far shows that the mucus in children with bronchiectasis is like that found in adults with bronchiectasis but overall is milder. The severity of hyperconcentration can also be quite variable. These findings are encouraging because there may be a window of opportunity to intervene and prevent further changes and either reverse or prevent permanent airway damage (i.e. bronchiectasis).
If you want to know more about bronchiectasis – take a look at the Bronchiectasis toolbox.
Respiratory Care Nurses
Find support that can help you better understand or manage living with a chronic lung condition like bronchiectasis. Lung Foundation Australia’s respiratory care nurse service can support individuals, families and carers with evidence-based guidance across all aspects of their condition. Book an appointment
For further information visit Lung Foundation Australia.
